How Safe is Ibogaine? We Asked Clare Wilkins Who Has Facilitated Over 700 Treatments | Part 9
Using ibogaine can be fatal if proper safety precautions aren’t taken. Read the full series.
Psymposia is a 501(c)(3) nonprofit research and media organization that offers critical perspectives on drugs, politics, and culture. We rely on contributions from our readers and listeners. Your support is vital to sustaining Psymposia.
Support Psymposia’s independent journalism on Patreon and help us drive the Mystery Machine! We’re a bunch of meddling kids who are unmasking the latest shenanigans on the psychedelics beat.
Clare S. Wilkins is a former intravenous drug user & methadone patient who shed her chemical dependencies with the aid of ibogaine. As founder of Pangea Biomedics, she has facilitated over 700 treatments and collaborated with MAPS on the Mexico study. Since 2010, Clare has been an active board member of the Global Ibogaine Therapy Alliance (GITA) and is a co-author of the Clinical Guidelines for Ibogaine-Assisted Detoxification. Clare is currently collaborating with ICEERS, developing a clinical trial for methadone for ibogaine-assisted detox.
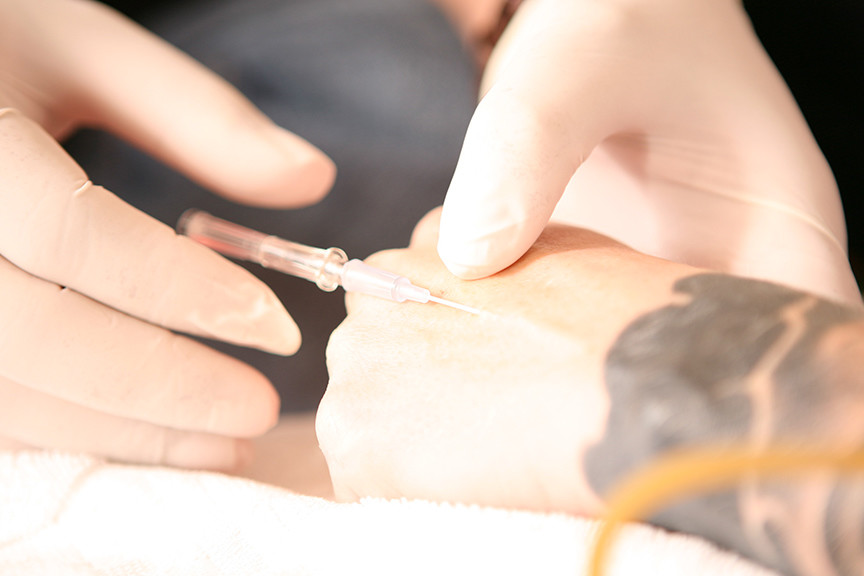
We’ve mentioned that ibogaine can be dangerous, and we even saw what can happen when proper safety precautions aren’t taken. Here, we take some time to speak with Clare and go more in depth about the risks associated with ibogaine.
While we hope that this interview offers some insight about the safety protocols one should consider before taking ibogaine, we want to stress that in no way should this be considered a thorough safety guide. Simply reading this interview is not adequate preparation, and we strongly encourage anyone thinking about working with ibogaine in any capacity to take the time to do further research.
Would you like to start us off by introducing yourself? What’s your story?
I was an injecting heroin user before switching to methadone. I come from a very traumatic childhood with a lot of violence. I discovered heroin at an Ivy League university, and it seemed to answer every question I ever had.
I spent the next 15 years trying to resolve that answer.
Methadone maintenance treatment worked for a while. It was my lily pad for 9 years. It saved my life. It made me not a criminal, not sick. I had a job, and I was able to get my life together.
Anyway, my sister and I had both been using heroin and she had already detoxed, yet she learned about iboga through Rick Strassman’s work with DMT. It was back when there were just a few clinics in the world. I went to a clinic in Tijuana, which, at that time, was the Ibogaine Association. There, I was freed from the lock of methadone.
After my experience, I saw what may have been lacking in the treatment protocol. I didn’t really have anybody to process with during the experience. I went home, and I was in withdrawal for a month. I couldn’t even do my job. So, I called up the clinic and told them that I’d like to talk to patients who perhaps needed to understand the process from a peer perspective. I was in LA and they were in Tijuana, so I’d take the train down and I’d just sit with people because no one who had taken ibogaine had ever sat with me.
That was the beginning. I volunteered until I was brave enough to purchase the Ibogaine Association name and create Pangea with a full team in a new location. It was a calling, and it seems to be a calling that happens with a lot of people in the drug users’ movement.
Since then, you’ve become prominent in the ibogaine community as a provider and consultant. In your professional opinion, is ibogaine actually safe?
That’s like asking if electricity is safe, in my opinion. You can cook a warm meal, light up a room, or electrocute someone with electricity, as they say.
It’s similar with ibogaine. Ibogaine, in and of itself, is not unsafe. There are both risks and benefits.
Ken Alper, Jeffrey Kamlet, Deborah Mash, Bruno Rasmussen, Roman Paskulin, and Jamie McAlpin are doctors and experts regarding ibogaine safety. There are many published journal articles and presentations of theirs online. To be clear, I’m a lay therapist that’s worked with an integrative team of MDs, naturopathic doctors, psychiatrists, psychologists, and somatic and peer therapists for 12 years.

So, what are some of the specific risks? You mentioned the heart, but could you go into detail about the screenings people should get before they consider taking ibogaine?
Ibogaine increases electricity in the heart, which is one of the reasons reputable clinics do cardiac screenings – to assess how the heart conducts electricity. Ibogaine has some features that require vigilance, and most experts conclude that thorough pre-screening and medical monitoring during the experience is crucial to its safety as a treatment for detoxification.
Ibogaine also induces bradycardia (it lowers heart rate, normally by about 10 beats per minute during a typical dose of 12 – 20mg/kg). The risk of bradycardia is that the heart rate can go very low. If the heart rate stays too low for too long of a period, this can require immediate administration of atropine. This is a serious life-threatening situation that requires medical intervention.
QT prolongation is another major risk with ibogaine. The QT interval is a measure of the heart’s electrical cycle, or the time it takes for the ventricle to get ready from one contraction to the next. During this period, the heart is vulnerable to cardiac arrhythmias and other serious complications. Other legal medications prolong the QT interval, such as methadone. Benzodiazepine and alcohol withdrawal both result in QT prolongation as well, so combining ibogaine with an alcohol or benzodiazepine detox can be extremely dangerous.
Many people who seek out ibogaine for detoxification are poly-drug users. For best outcomes, complete blood and urine panels need to be drawn and analyzed as close to treatment as possible to assess for infection, electrolyte levels, and of course, a toxicology screen. What drugs/medications has this person been taking that they may not have told you about?
Hepatic function and the specific liver enzymes are essential. Many ibogaine patients have liver issues, are diagnosed with hepatitis C, etc. However, this doesn’t preclude them from treatment, in many providers’ experience. Still, the liver enzyme count is crucial to consider. I believe Howard Lotsof’s last patent application was for the use of ibogaine to treat hepatitis C. He had data demonstrating a dramatic decline in viral load counts in those with a diagnosis of Hepatitis C who had taken ibogaine.
Electrolyte count is crucial as well because ibogaine is a potassium hERG channel blocker. Potassium plays an important role in cardiac function, and blocking this channel can lead to prolonged QT intervals, arrhythmias, and insufficient electrolytes for the heart to function as it needs to.
Noribogaine, the metabolite of ibogaine, is an important topic as well. It seems to stay in the system longer than ibogaine, providing the “window of opportunity” we hear about. Noribogaine has similar qualities to ibogaine in terms of decreased self-administration of opiates. According to Ken Alper and others, it’s important to consider the concentration of noribogaine over time, which resembles a curve. Multiple doses of ibogaine in one evening increase the area under the curve, indicating a higher concentration of noribogaine in the system for longer periods of time, which could or could not be predictive of more danger.
In your time as a provider, did you ever have any adverse events?
Pangea had 3 fatalities, on separate occasions, as well as numerous events that required intervention. Thanks to mentors, experts, and teachers, Pangea learned from them. We haven’t had an adverse event since because we do completely different protocols now that have been worked on diligently for the past 8 years.
We don’t just pull the rug right out from under the client upon starting treatment. No need to arrive in withdrawal. Before treatment, we develop specific protocols to treat conditions underlying their dependencies. We continue with this process during treatment.
Our work with ibogaine is done in a specifically timed manner. For example, with opioid dependencies, we give morphine and then ibogaine, then less morphine, and then ibogaine. As the ibogaine accumulates, there’s less and less craving for opioids, and more time to include the adjunct therapies we use. With stimulants, we don’t use the method of co-administration, yet we do use repeated cumulative dosing. It takes an extreme amount of vigilance, but it’s much more successful than anything we ever did before while following the traditional model.
Why did these adverse events occur?
Well first, we were following the traditional model. In the conventional paradigm, you come to treatment in withdrawal and you get ibogaine that night, before trust is developed with the team, soon after an EKG, and usually after a long flight.
We had a staff of 12, including 4 doctors. We essentially had a hospital in a villa; it wasn’t for a lack of equipment or personnel. These were extremely unfortunate and difficult aspects of the learning curve. The fatalities were the result of pulmonary embolism, the presence of residual cocaine in the blood, and hypertrophy. All preventable issues, as we now know.
So, do you think your current model helps prevent adverse events?
Not think, we know.
No deaths and no hospital visits in the 8 years since we have changed our protocols. We’ve had someone who experienced a hypertensive attack, who already had high blood pressure, and we controlled it within an hour. And someone else was vomiting so much they needed an IV, but that would happen almost every week when we administered ibogaine the previous way.
Psychologically, it’s a different story. Clients can regress to their childhoods, start acting child-like, screaming, crying, or behaving violently. Staying in an alternate reality for a prolonged period of time, this comes with safety issues as well.
What’s so different about this alternative protocol?
Well, the traditional treatment model is rapid. Patients come in, they take their ibogaine, and they usually return to their same environment shortly after treatment.
We now emphasize pre-treatment at least a month before they come. Many people focus on aftercare, but nobody seems to talk much about strong preparatory care.
We’ve had numerous clients follow our preparatory protocol who end up not needing to take ibogaine. We worked with naturopaths and developed specific orthomolecular protocols for the 5 most significant physiological issues that occur with drug dependence. Those are depression, pain, anxiety, liver issues, and chronic fatigue.
What we do is called repeated cumulative low dosing, which results in a saturation, or a “flood”, by the end. So instead of giving a single flood dose in one night, we do it over days. What that does is it shows us how someone reacts to the medicine, how they metabolize the drug – versus just going from a blood test result. So how do they react at first? Do they cry? Do they feel nothing? Do they say it feels good? Do they see their dead grandparents? Do they feel calm or anxious at first? Then, as a team, we form a specific protocol based on their body and mind. They teach us.
Is ibogaine safe to take with any other medications?
There are many contraindications. Ibogaine potentiates not just morphine, but it seems to be a potentiator of almost everything. One cup of coffee with a microdose of ibogaine in the morning can feel like 4 cups to some people. Antidepressants and antipsychotics are another category that are restricted with ibogaine. I highly suggest people do a lot of research regarding this issue, as it could take a while to go through all the medications. The GITA Guidelines have information as well.
Working with a physician who supports the use of ibogaine and tapering from other medications, or continued use of them, is strongly encouraged.
It seems like there’s a lot of controversy and misinformation surrounding ibogaine and benzos. What’s the deal? Is it safe to detox from benzos using ibogaine?
Ibogaine doesn’t work as well for benzos as it does for opioids and stimulants.
Remember, ibogaine electrifies the body. Yes, with the correct dose it can place a person into a para-sympathetic state, where he or she is no longer in fear. Yet it’s extremely dangerous to use ibogaine to decrease the dosage of a benzo, especially rapidly. We refer people to the Ashton manual. Heather Ashton is the world’s expert on benzo tapering.
Of course, one can combine various therapies to detox from benzodiazepines, but we’ve seen that a slow taper, over time, is the safest with long-acting benzodiazepines. Withdrawal from benzos includes QT prolongation, anxiety, fear, insomnia, seizures, and even death. When a person who is dependent on benzos takes ibogaine, they need to be stabilized on a long-acting benzo to keep the QT interval in a safe range. A short acting benzodiazepine can leave the system during a “flood” quickly, increasing the risk of seizures and arrhythmias. It can also stay in the system and be potentiated by the ibogaine.
This all depends on an individual’s body and their metabolism, as well as dosage of the benzos. We don’t know unless we go slowly. There’s debate around this issue, so it would be wonderful if the clinics who work well with benzodiazepine patients can come together and share their knowledge with other providers and patients.
Many people hide their benzo use, even if it’s only occasional, to be accepted to clinics, and this is dangerous. If you look at Ken Alper’s fatality paper, you’ll see benzodiazepines are connected to many of the deaths associated with ibogaine – specifically you’ll see that they weren’t used while in treatment, yet were found in the toxicology report afterward. I call benzos the snipers of ibogaine fatalities.
This subject is controversial because you have a doctor saying one thing and a clinic saying another thing, and so on.
How about other psychedelics? That seems to be a growing trend, taking ibogaine with other visionary substances. How safe is this?
Ibogaine is safe to take with certain psychedelics. And completely unsafe with others.
Dangers seem to occur around the administration of 5-MeO-DMT, kambo, MDMA, and ayahuasca in close proximity with ibogaine. There have been grievances, including a fatality, associated with the use of these medicines alongside ibogaine.
Ayahuasca and kambo are both purgatives, so the issues of dehydration and over-stimulation can be factors in relation to safety with ibogaine treatment. There’s been a surge of the use of these medicines with one another in the past few years. A few practitioners seem to combine the higher risk substances well, with no adverse effects reported. There’s a lot that still needs to be researched.
There’s also debate around using ketamine, which is a dissociative, while taking ibogaine or shortly after. Many clinics have witnessed clients moving from heroin/opioids to ketamine after taking ibogaine, and from stimulants to 5-MeO-DMT and/or DMT as a form of psychedelic substitute. Aside from the physiological complications that may arise from these combinations, there is the psychological component.
Experiences with certain substances can take months, or more, to fully integrate. Often, ibogaine is not enough to get the mission accomplished on its own, to treat years of a chronic condition. It’s essential to use adjunct therapies to create an integrative experience for the client. This, of course, takes time.

A lot of people are talking about microdosing ibogaine. Are the risks the same as with a larger threshold dose? Should someone still get screened before starting a microdosing regimen?
The risks can be the same, yes. They are far less significant, of course, because the dose is so much smaller than traditional “flood” doses.
Yet, there are people who just simply cannot and should not take ibogaine, period.
Even small doses can exacerbate a heart condition, anxiety, or insomnia. Ibogaine is cumulative, so as it builds up (if you’re microdosing regularly), it eventually saturates the body and it feels like you’ve taken a larger amount that day than you actually have. I know of people who used it daily, with a day of rest per week, and others who had a panic attack with a first dose of only a few milligrams. Although not a microdose, a fatality occurred recently with a dose of only 200mg ibogaine HCl, which is considered less than a “booster dose.”
It’s important to rest, to integrate, to sleep, to dream, and to allow the cascade effect of ibogaine to work its wonders. A guide or facilitator is highly recommended. Others prefer finding their own inner guide – their inner doctor, so to speak. Ibogaine leads us back to the root of our inner voice, which we lose sometimes in this cacophony of modern life.
It seems like there’s a lot of misinformation out there surrounding ibogaine, specifically regarding safety protocol. What do you think are some of the most common misconceptions people have about ibogaine in general?
That they will be liberated from addiction for life. That they will understand the root causes of their dependencies and be able to easily move forward from those realizations. That they’re able to integrate their experience back into their regular life, like it’s easy peasy from there on.
A myth is that everything is fine and perfect after it’s over. With ibogaine, yeah in a night, over the course of a few hours, you’ll be devoid of most withdrawal symptoms and cravings. But after that is when the real work begins.
Those are some of the main ones. Most people don’t know how to integrate what happened to them while taking ibogaine into their life. It’s tough. That’s why if you look on our website, we have a page called ‘The Family’. The family is an organism, and if we notice a family member doesn’t want to talk and be included in therapy, we start to understand that the user may be the scapegoat. Dependency is a family issue that’s complex to traverse.
So all in all, would you say ibogaine is worth taking even despite the safety risks?
Ibogaine is for the person who feels called to it, who resonates with it, just as you do with a food, a country, a friend, a plant, a potential lover, an ally.
One can feel more of the world around them after taking ibogaine, see more clearly, and experience a new awareness of themself that grows or suddenly appears.
We need more people who feel right now. Who see more deeply. It’s urgent. The risk is worth it.
It certainly has been for me.
Read Part 10: Ibogaine treatment comes with risks. We had a discussion about safety with medical providers.
Hey! Before you go… Psymposia is a 501(c)(3) non-profit media organization that offers critical perspectives on drugs, politics, and culture. We strive to ask challenging questions, and we’re committed to independent reporting, critical analysis, and holding those who wield power accountable.
Our perspectives are informed by critical analysis of the systemic crises of capitalism that have directly contributed to the unmitigated growth of addiction, depression, suicide, and the unraveling of our social relations. The same economic elite and powerful corporate interests who have profited from causing these problems are now proposing “solutions”—solutions which both line their pockets and mask the necessity of structural change.
In order for us to keep unpacking these issues and informing our audience, we need your continuing support. You can sustain Psymposia by becoming a supporter for as little as $2 a month.
Jordan May
Jordan May is a writer who explores the intersections between drug policy, psychedelics, and community engagement.





